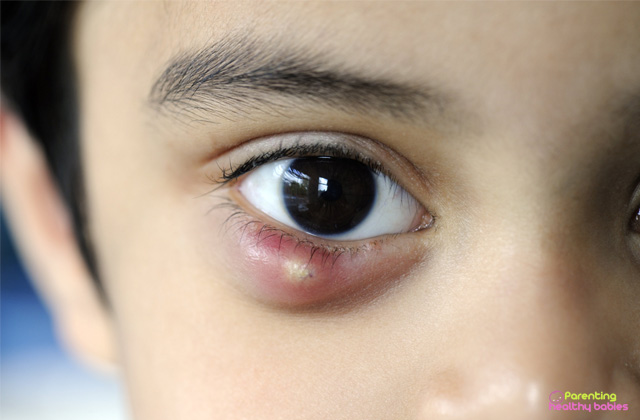
Periorbital cellulitis, also known as preseptal cellulitis, is a bacterial infection that affects the eyelids and surrounding skin. It is most commonly seen in children and can lead to serious complications if not treated promptly. The condition is characterized by inflammation, redness, and swelling around the eye, and it typically results from a local infection or trauma. Understanding the causes, symptoms, treatment options, and potential complications is crucial for effective management and prevention of further issues.
In This Article:
- Causes of Periorbital Cellulitis
- Symptoms of Periorbital Cellulitis
- Treatment for Periorbital Cellulitis
- Orbital Cellulitis Stages
- Periorbital Cellulitis NHS Guidelines
- Is Periorbital Cellulitis an Emergency?
- Is Periorbital Cellulitis Contagious?
Periorbital cellulitis differs from orbital cellulitis, which involves deeper structures within the orbit and can lead to more severe consequences. Early diagnosis and treatment are essential to prevent the infection from spreading and to ensure a full recovery.
Causes of Periorbital Cellulitis
Bacterial Infections:
Periorbital cellulitis is usually caused by bacterial pathogens such as Staphylococcus aureus and Streptococcus pyogenes. These bacteria can invade the skin around the eye through cuts, insect bites, or other breaks in the skin.
Sinusitis:
Infections in the sinuses, particularly the ethmoid sinuses, can spread to the periorbital area, leading to cellulitis. This is more common in children due to their closer anatomical proximity.
Trauma:
Injuries or trauma to the area around the eye, including minor cuts, scratches, or insect bites, can provide an entry point for bacteria, leading to infection.
Dental Infections:
Severe dental infections can sometimes spread to the facial tissues, including the area around the eye, causing periorbital cellulitis.
Upper Respiratory Infections:
Infections such as colds or flu can increase the risk of developing periorbital cellulitis, especially if the infection spreads to the sinuses.
Skin Conditions:
Pre-existing skin conditions like eczema or dermatitis can break down the protective barrier of the skin, making it easier for bacteria to penetrate and cause infection.
Immunocompromised State:
Children with weakened immune systems, due to conditions like diabetes or immune deficiencies, are at higher risk for developing periorbital cellulitis.
Foreign Bodies:
The presence of a foreign body in the eye, such as a splinter or sand particle, can introduce bacteria and cause infection in the surrounding tissue.
Symptoms of Periorbital Cellulitis
Swelling:
One of the most noticeable symptoms of periorbital cellulitis is swelling around the affected eye, which can make the eyelid appear puffy and distended.
Redness:
The skin around the eye often becomes red and inflamed, indicating the presence of infection and inflammation.
Pain and Tenderness:
The area around the eye may become painful and tender to touch, with discomfort increasing during activities such as blinking or movement.
Fever:
Children with periorbital cellulitis may develop a fever as the body’s immune system responds to the bacterial infection.
Eye Discharge:
In some cases, there may be discharge from the eye, which can be clear, yellow, or green, depending on the severity of the infection.
Visual Disturbances:
Although less common, severe swelling can sometimes cause visual disturbances or a feeling of pressure in the eye.
General Malaise:
Children may feel generally unwell, with symptoms such as fatigue, irritability, and loss of appetite.
Reduced Eye Movement:
In cases where the infection spreads or becomes severe, there may be noticeable limitations in the movement of the eye, indicating a need for immediate medical attention.
Treatment for Periorbital Cellulitis
Antibiotics:
The primary treatment for periorbital cellulitis is antibiotics, which can be administered orally or intravenously, depending on the severity of the infection. Common antibiotics used include amoxicillin-clavulanate and cefuroxime.
Warm Compresses:
Applying warm compresses to the affected area can help reduce swelling and provide comfort. It also aids in improving blood flow, which can help in the healing process.
Pain Management:
Over-the-counter pain relievers such as acetaminophen or ibuprofen can help manage pain and reduce fever associated with periorbital cellulitis.
Monitoring for Complications:
Close monitoring is essential to detect any signs of the infection spreading to deeper tissues, which may require more aggressive treatment or hospitalization.
Hospitalization:
In severe cases, particularly where there is a risk of the infection spreading to the orbit or causing systemic issues, hospitalization may be required for intravenous antibiotics and close monitoring.
Surgery:
Rarely, if there is an abscess or if the infection does not respond to antibiotics, surgical intervention may be necessary to drain the infected area and prevent further complications.
Follow-Up Care:
Regular follow-up appointments are important to ensure that the infection has been completely resolved and to monitor for any signs of recurrence.
Prevention:
Preventative measures include maintaining good hygiene, treating underlying conditions like sinusitis promptly, and protecting the eye area from injury or trauma
Orbital Cellulitis Stages
- Preseptal Cellulitis: This stage is characterized by infection confined to the eyelid and surrounding skin, not extending beyond the orbital septum. It is less severe and easier to treat compared to deeper infections.
- Early Orbital Cellulitis: The infection starts spreading beyond the septum into the orbit, leading to more pronounced symptoms such as significant swelling, redness, and pain, as well as possible visual disturbances.
- Orbital Abscess Formation: If left untreated, the infection can progress to form an abscess within the orbital tissues. This stage is marked by increased swelling, pain, and a higher risk of vision loss and other serious complications.
- Cavernous Sinus Thrombosis: In severe cases, the infection can spread to the cavernous sinus, a large vein located at the base of the brain. This stage can lead to life-threatening complications, including brain abscesses and meningitis.
- Systemic Spread: The final and most dangerous stage involves the infection spreading beyond the orbit into the bloodstream, leading to sepsis and potential systemic failure.
- Diagnosis and Intervention: Early diagnosis and intervention at any stage are crucial to prevent progression and serious outcomes. Imaging studies like CT scans and MRIs are often used to assess the extent of the infection.
- Treatment at Different Stages: Treatment varies depending on the stage, ranging from antibiotics for early stages to surgical drainage for abscess formation and aggressive systemic treatment for advanced stages.
- Recovery and Follow-Up: Recovery involves close monitoring, particularly in advanced stages, to ensure complete resolution and to prevent recurrence or long-term complications.
Periorbital Cellulitis NHS Guidelines
- Early Recognition: The NHS emphasizes the importance of early recognition of periorbital cellulitis symptoms to prevent complications. Prompt identification and treatment are critical.
- Clinical Assessment: A thorough clinical assessment, including a review of medical history and physical examination, is recommended to confirm the diagnosis and rule out other conditions.
- Antibiotic Therapy: The NHS guidelines recommend starting antibiotic therapy immediately, with options including oral or intravenous antibiotics depending on the severity of the infection.
- Hospitalization Criteria: Guidelines suggest hospitalization for children who are very young, show severe symptoms, or have comorbid conditions that could complicate the infection.
- Monitoring and Follow-Up: Close monitoring during and after treatment is advised to ensure the infection is resolved and to check for any signs of complications or recurrence.
- Referral to Specialists: In cases where the infection is not responding to initial treatment or if there are signs of orbital involvement, referral to an ophthalmologist or infectious disease specialist is recommended.
- Imaging and Diagnosis: Use of imaging techniques like CT scans may be necessary to assess the extent of the infection and to differentiate between periorbital and orbital cellulitis.
- Public Health Advice: The NHS provides public health advice on maintaining good hygiene and seeking prompt medical attention for symptoms suggestive of periorbital cellulitis to prevent spread and complications.
Is Periorbital Cellulitis an Emergency?
- Potential for Complications: Periorbital cellulitis can lead to serious complications if left untreated, including the spread of infection to the orbit or other parts of the body.
- Risk of Orbital Cellulitis: If the infection spreads beyond the eyelid to the orbit, it can lead to orbital cellulitis, which is a medical emergency requiring immediate attention.
- Need for Prompt Treatment: Prompt treatment with antibiotics is essential to prevent the infection from progressing and to minimize the risk of serious complications.
- Hospitalization Criteria: Severe cases, particularly in very young children or those with significant symptoms, may require hospitalization for intravenous antibiotics and close monitoring.
- Signs of Emergency: Symptoms such as worsening pain, vision changes, high fever, or inability to move the eye should be treated as emergencies and require immediate medical evaluation.
- Potential for Systemic Spread: The infection can potentially spread to the bloodstream, leading to sepsis, which is a life-threatening condition that requires urgent medical intervention.
- Follow-Up Care: Even after initial treatment, close follow-up is important to ensure the infection is fully resolved and to prevent recurrence.
- Differentiating from Other Conditions: It is important to differentiate periorbital cellulitis from other conditions like allergic reactions or insect bites, which may present similarly but do not require urgent antibiotic treatment.
Is Periorbital Cellulitis Contagious?
- Bacterial Nature: Periorbital cellulitis itself is not contagious; however, the underlying bacterial infections that can lead to the condition, such as strep throat or sinusitis, can be contagious.
- Spread Through Contact: While the infection around the eye is not spread from person to person, the bacteria responsible can spread through direct contact with infected secretions.
- Preventive Measures: Good hygiene practices, such as regular hand washing and avoiding touching the face, can help prevent the spread of bacteria that may lead to periorbital cellulitis.
- Secondary Infections: Infections that can precede periorbital cellulitis, such as sinus infections, can be spread to others, increasing the risk of subsequent complications.
- Isolation Precautions: Although periorbital cellulitis is not spread directly, children with the condition should be kept away from others to prevent the spread of the underlying bacterial infections.
- Hygiene Importance: Maintaining good hygiene, especially in childcare settings, is essential to minimize the risk of bacterial infections that could lead to periorbital cellulitis.
- Family Member Safety: Family members should practice good hygiene to prevent the spread of bacteria within the household, especially if someone has a bacterial infection.
- Vaccinations: Ensuring up-to-date vaccinations, such as those for Haemophilus influenzae type B and pneumococcus, can help prevent infections that might lead to periorbital cellulitis
Conclusion
Periorbital cellulitis in children is a serious bacterial infection that affects the tissues surrounding the eye. Prompt recognition and treatment are critical to prevent complications, such as the progression to orbital cellulitis or the spread of infection to other parts of the body. Understanding the causes, symptoms, and treatment options can help caregivers and healthcare providers manage this condition effectively.
Early intervention with appropriate antibiotics and supportive care can lead to a full recovery and prevent the need for more invasive treatments. While periorbital cellulitis itself is not contagious, the underlying bacterial infections that can lead to it are, highlighting the importance of good hygiene and preventive measures.
Ongoing education, awareness, and adherence to clinical guidelines are essential for reducing the incidence and impact of periorbital cellulitis in children. By staying informed and vigilant, parents and healthcare professionals can ensure the best outcomes for affected children and help prevent future occurrences of this potentially serious condition.
Sources:
- https://www.nhsinform.scot/illnesses-and-conditions/eyes/periorbital-cellulitis
- https://medlineplus.gov/ency/article/000978.htm
- https://www.mayoclinic.org/diseases-conditions/periorbital-cellulitis/symptoms-causes/syc-20355175
- https://kidshealth.org/en/parents/periorbital-cellulitis.html
- https://my.clevelandclinic.org/health/diseases/14607-periorbital-cellulitis